Major depressive disorder (MDD) continues to cast a long shadow over global public health, recognized as a significant contributor to disability worldwide. For a substantial portion of individuals diagnosed with depression, approximately 30%, standard antidepressant medications prove insufficient, leading to a challenging condition known as treatment-resistant depression (TRD). In recent years, ketamine has emerged as a beacon of hope, offering rapid antidepressant effects for those grappling with TRD. However, the precise mechanisms by which ketamine exerts its influence within the human brain have remained a complex puzzle, hindering efforts to optimize and personalize this promising therapeutic avenue.
A groundbreaking study, published in the esteemed journal Molecular Psychiatry on March 5, 2026, has significantly advanced our understanding of this intricate process. Led by Professor Takuya Takahashi of the Department of Physiology at Yokohama City University Graduate School of Medicine in Japan, the research team employed a cutting-edge positron emission tomography (PET) imaging technique to directly observe the dynamic changes in glutamate α-amino-3-hydroxy-5-methyl-4-isoxazole propionic acid receptors (AMPARs). These critical protein receptors play a pivotal role in mediating communication between brain cells, underpinning synaptic plasticity and glutamatergic signaling, processes central to the therapeutic action of ketamine in patients with TRD.
"Despite ketamine’s demonstrated rapid antidepressant effects in patients with treatment-resistant depression, its molecular mechanism within the human brain has eluded complete clarification," stated Professor Takahashi, underscoring the long-standing scientific quest to demystify ketamine’s action. This latest research represents a significant leap forward in that endeavor.
Visualizing Brain Receptors with a Novel PET Tracer
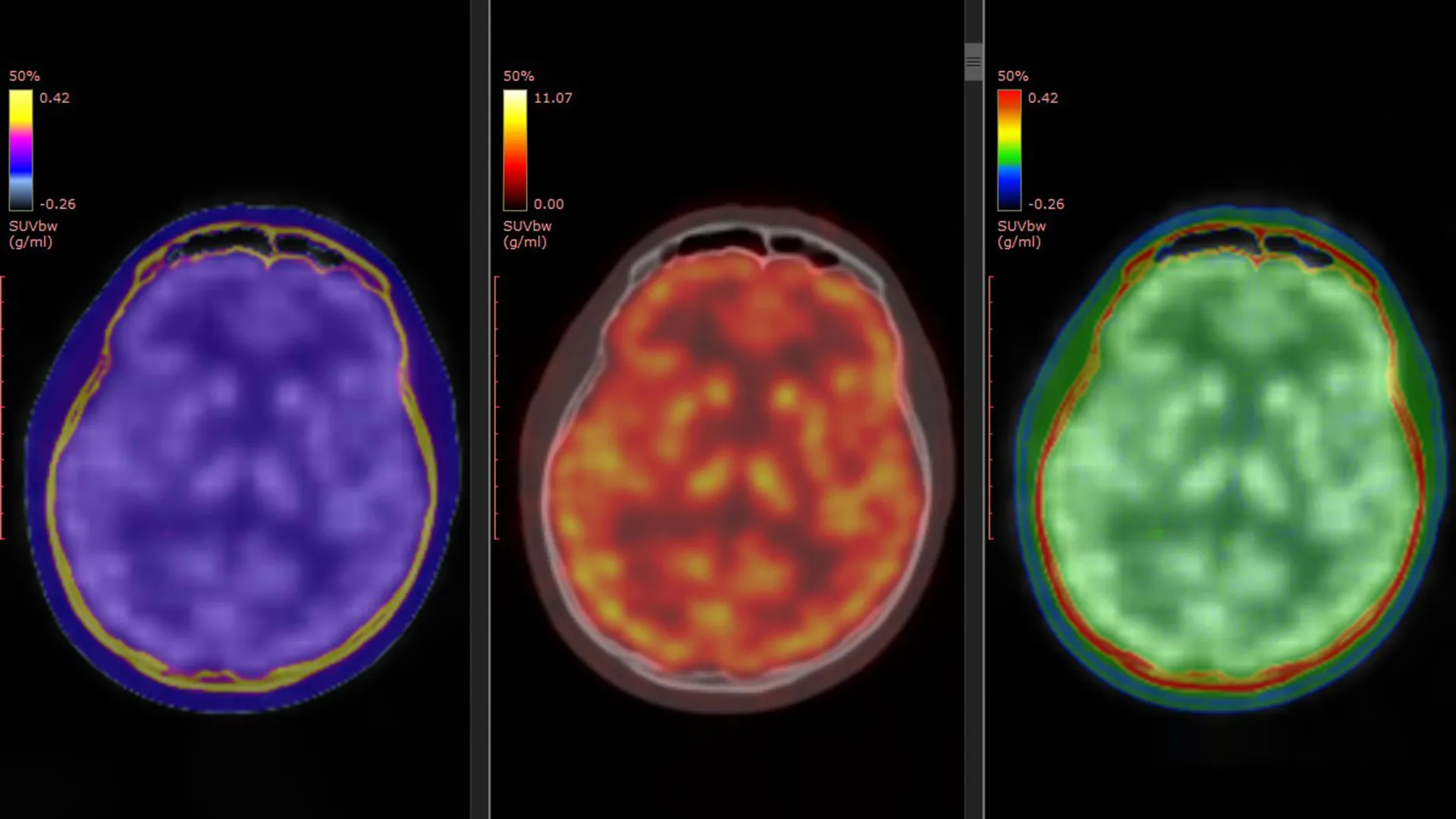
The cornerstone of this pivotal study was a novel PET tracer, designated as [¹¹C]K-2, developed by Professor Takahashi’s team. This sophisticated tracer possesses the unique capability to visualize cell-surface AMPARs directly within the living human brain. Prior laboratory and animal investigations had strongly suggested a role for AMPAR activity in mediating ketamine’s antidepressant effects. However, this new research provides the first direct, empirical evidence of this intricate biological process occurring in humans.
The study’s methodology involved a meticulous integration of data drawn from three registered clinical trials conducted in Japan. The cohort comprised 34 patients formally diagnosed with TRD and 49 healthy individuals who served as a crucial control group. This carefully designed comparison allowed researchers to isolate and observe the specific effects of ketamine on AMPARs in the context of depression.
Over a two-week period, participants received either intravenous ketamine or a placebo. PET brain imaging was conducted at two key junctures: prior to the commencement of treatment and again following the final infusion. This longitudinal imaging approach was instrumental in enabling researchers to precisely track and compare alterations in AMPAR levels and their distribution within the brain throughout the course of the intervention.
Region-Specific Brain Changes Linked to Symptom Relief
The findings revealed a compelling picture of brain activity. Individuals diagnosed with TRD exhibited widespread abnormalities in AMPAR density when contrasted with their healthy counterparts. Importantly, these differences were not uniformly distributed across the entire brain but were instead localized to specific neural regions. This suggests a targeted disruption in brain circuitry rather than a generalized deficit.
Furthermore, the study demonstrated that ketamine did not induce uniform changes in AMPAR density throughout the brain. Instead, the observed improvements in depressive symptoms were intrinsically linked to dynamic, region-specific adjustments in AMPAR levels. In certain cortical areas, there was an observed increase in AMPAR density, suggesting enhanced synaptic function. Conversely, reductions in AMPAR density were noted in brain regions critically involved in reward processing, most notably the habenula. The precise correlation between these region-specific shifts in AMPAR distribution and the amelioration of patients’ depressive symptoms was found to be statistically significant, highlighting a direct mechanistic link.
"Ketamine’s antidepressant effect in patients with TRD is mediated by dynamic changes in AMPAR in the living human brain," Professor Takahashi reiterated, emphasizing the significance of these in-vivo observations. "Using a novel PET tracer, [¹¹C]K-2, we were able to visualize how ketamine alters AMPAR distribution across specific brain regions and how these changes correlate with improvements in depressive symptoms." These findings offer robust human evidence that corroborates previously identified mechanisms from animal studies and, crucially, connects these molecular processes to tangible clinical antidepressant outcomes.
Potential Biomarker for Predicting Treatment Response
Beyond clarifying the intricate molecular pathways of ketamine’s action, these findings hold significant promise for practical clinical application. The ability to visualize AMPAR density using PET imaging could potentially evolve into a valuable biomarker. Such a biomarker could empower clinicians to more accurately evaluate and predict an individual’s response to ketamine treatment for TRD.
The persistent challenge of identifying reliable biological markers for treatment response remains a critical unmet need in mental health care, particularly given the significant proportion of patients who do not achieve adequate relief from standard antidepressant therapies. The development of AMPAR PET imaging as a predictive tool could revolutionize the management of TRD by enabling more informed treatment decisions and reducing the trial-and-error approach often associated with current therapeutic strategies.
Toward More Personalized Depression Treatments
This research represents a crucial step in bridging the long-standing gap between fundamental laboratory discoveries and their translation into effective clinical psychiatric practice. By enabling scientists to directly observe AMPAR activity in the living human brain, the study provides concrete evidence that AMPAR modulation is a central mechanism underlying ketamine’s rapid antidepressant effects. This insight paves the way for the development of more personalized and precise treatment strategies for individuals living with treatment-resistant depression.
The implications of this work extend beyond the immediate understanding of ketamine. It opens avenues for the investigation of other glutamatergic modulators and their potential in treating depression. The ability to visualize specific receptor dynamics could accelerate the discovery and development of novel therapeutics tailored to the unique biological profiles of individual patients. Ultimately, this research is poised to foster the creation of more targeted and effective interventions, offering renewed hope to the millions worldwide affected by the debilitating effects of treatment-resistant depression.
The study was generously supported by funding from various esteemed institutions, including the Ministry of Education, Culture, Sports, Science and Technology (Special Coordination Funds for Promoting Science and Technology); the Japan Agency for Medical Research and Development (AMED) (grant numbers: JP18dm0207023, JP19dm0207072, JP24wm0625304, JP25gm7010019, and JP20dm0107124); the Japan Society for the Promotion of Science KAKENHI (grant numbers: 22H03001, 20H00549, 20H05922, 23K10432, 19H03587, 20K20603, 22K15793, and 21K07508); the Takeda Science Foundation; the Keio Next-Generation Research Project Program; the SENSHIN Medical Research Foundation; and the Japan Research Foundation for Clinical Pharmacology. This broad base of support underscores the recognized importance and potential impact of this critical research.







