The Medicines and Healthcare products Regulatory Agency (MHRA) has initiated a sweeping investigation into numerous UK clinics, probing whether they are in breach of the law by promoting experimental, unregulated peptide therapies with unproven medicinal claims. This significant move, revealed through a Guardian investigation, underscores growing concerns about the proliferation of unverified health and wellness treatments and the potential risks they pose to public safety.
The Rise of Experimental Peptides and Regulatory Scrutiny
In recent years, interest in experimental peptide therapies has witnessed an exponential boom, fueled by a burgeoning wellness industry and widespread promotion across social media platforms. These substances, typically administered via injection, are marketed by clinics, influencers, and even some medical practitioners as panaceas for a diverse range of conditions, from enhancing anti-ageing processes and accelerating injury recovery to boosting cognitive function and improving metabolic health. However, this surge in popularity has far outpaced the scientific evidence, with robust human clinical trials largely absent. The vast majority of studies supporting these claims have been conducted in animals or isolated cells, rendering their applicability and safety in humans highly questionable.
The MHRA has explicitly stated that clinics are not permitted to make medicinal claims for peptide treatments unless those products have undergone the rigorous authorisation process required for licensed medicines. An MHRA spokesperson confirmed the agency’s firm stance: “If clinics offering peptide injections make medicinal claims for those treatments, the products will be considered medicines and subject to regulation under the Human Medicines Regulations 2012. The MHRA will take action against clinics which are identified as breaching the legal requirements.” This regulatory framework is designed to protect public health by ensuring that all medicines meet stringent standards for safety, quality, and efficacy before they can be marketed for therapeutic use.
Guardian Investigation Uncovers Widespread Non-Compliance
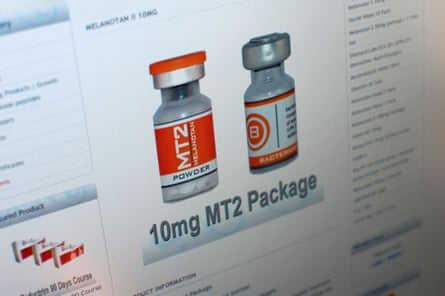
A comprehensive investigation by the Guardian has brought to light a significant number of clinics operating across the UK that are openly offering a variety of unregulated, experimental peptides and making extensive, unverified claims about their purported benefits directly on their public-facing websites. This journalistic deep dive exposed a systemic issue where commercial interests appear to be overriding regulatory guidelines and scientific principles.
One prominent example identified was a clinic appearing high in Google search results for "peptide clinics UK." Its website brazenly advertised specific peptides with explicit medicinal claims: Cortexin was stated to be "used for neuroprotection and cognitive enhancement," BPC-157 as aiding "tissue repair and recovery from injuries," and Thymosin Alpha as boosting "immune function." The MHRA unequivocally confirmed that such statements constituted medicinal claims for unauthorised treatments and were, therefore, illegal. Following direct contact from the Guardian for comment, the clinic promptly removed these problematic claims from its website, highlighting the immediate impact of journalistic scrutiny and the underlying awareness of regulatory violations.
Another top-ranked clinic presented a more nuanced, yet still concerning, approach. While acknowledging on its website that peptides "are lacking large clinical trials" and stressing that "human evidence is limited," it paradoxically proceeded to advertise seven named peptides, complete with "results duration" and pricing for each. This was done despite explicitly labelling them as "research only," a clear attempt to navigate regulatory boundaries while still enticing consumers with therapeutic promises. The pricing structure revealed the significant financial investment requested from clients, with a single peptide costing £350 per month and two peptides priced at £450 per month. These therapies were offered in vials with disposable syringes or, for an additional fee, in pre-loaded injection pens, indicating a professionalised delivery model for what are essentially unregulated substances.

The Consultative Experience: Blurring Lines and Undisclosed Risks
To further understand the operational practices of these clinics, a Guardian reporter undertook a free consultation with one of the identified establishments. During this consultation, the clinician did acknowledge that "most research into peptides was pre-clinical and some peptides were still very experimental." They also conceded that "there was a lack of randomised multi-centre clinical trials for peptides to provide information about their long-term effects." This transparency, however, was juxtaposed with a clear promotional agenda. The clinician advised a periodic break of "four to eight weeks off between two to three month periods of using a peptide to reduce any risks," a recommendation devoid of robust clinical backing for these specific experimental compounds.
Despite the stated limitations, the clinician proceeded to recommend two peptides to the reporter: BPC-157 and MOTS-C, to aid with recovery after exercise and fatigue. The descriptions of their benefits, while couched in cautious language, still leaned heavily towards medicinal claims.
-
BPC-157: Described as "one of the more commonly used peptides," the clinician stated: "It helps in repair and recovery of cells. So if somebody comes to us saying I want to get fitter, lift heavier, get bigger muscle, I will still recommend BPC-157, even though it doesn’t directly affect any of those things. It’s because it helps your recovery after those workouts." They further elaborated, "This helps provide more blood flow and nutrients to different tissues that need repair… [and] promotes quicker recovery from whatever physical activity that you’ve done." Alarmingly, the clinician also noted a significant health caveat: BPC-157 was "not advised for people who smoke or have a family history of cancer as there were concerns the peptide could increase blood supply to such tissue and help fuel the cancer." This stark warning underscores the profound and potentially life-threatening risks associated with unproven substances, where even practitioners acknowledge serious contraindications based on limited data.
-
MOTS-C: The second recommended peptide, MOTS-C, was presented with a cascade of purported metabolic benefits. The clinician claimed: "MOTS-C is something that helps provide more stress resilience and better health to your mitochondria to be able to produce more energy cells… so the direct net effect for you would be reduced insulin resistance, better energy production in the form of [the energy molecule] ATP, and the net result of that is basically reduce visceral fat." These claims, linking MOTS-C to fundamental cellular processes and tangible health outcomes like fat reduction, undeniably fall under the umbrella of medicinal claims.
The MHRA has confirmed that it is actively investigating whether the claims made by the clinician during this consultation also constitute unlawful medicinal claims. The clinic, in its defence, maintained that it had "clearly explained that the peptides discussed are not licensed medicines, and that the current evidence base is largely pre-clinical, with an absence of large-scale randomised controlled trials assessing long-term outcomes." It asserted that its consultations encouraged "shared decision-making, where individuals are given balanced information on potential mechanisms, theoretical benefits and uncertainties." However, the juxtaposition of these disclaimers with specific recommendations and descriptions of therapeutic outcomes raises serious questions about the practical application of "shared decision-making" when the fundamental scientific backing is absent.
A spokesperson for the clinic further argued for the necessity of their services, stating that it was "important to acknowledge the current reality: a significant number of individuals in the UK are already accessing peptide products through unregulated channels (including informal online networks such as messaging platforms), where there is little to no clinical oversight, quality assurance, or safety screening." While this highlights a broader challenge in the unregulated market, it does not absolve regulated clinics from adhering to established medical and legal standards.
Understanding Peptides: The Scientific Context
Peptides are short chains of amino acids, the building blocks of proteins. Many occur naturally in the human body, playing crucial roles as hormones, neurotransmitters, and growth factors. A well-known example is insulin, a naturally occurring peptide hormone vital for regulating blood sugar levels. In recent decades, scientific advancements have enabled the synthesis and study of numerous peptides for therapeutic purposes.
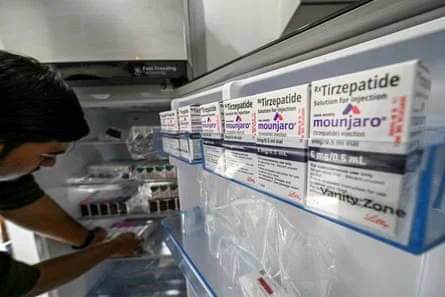
This research has led to the development of genuinely transformative, approved prescription medications based on synthetic peptides. Notable examples include semaglutide (found in weight-loss drugs like Wegovy) and tirzepatide (found in Mounjaro), which mimic natural hormones to regulate appetite and metabolism. These drugs have undergone extensive, multi-phase clinical trials, demonstrating their safety and efficacy under strict regulatory oversight before being made available to patients.
However, the vast majority of peptides currently marketed by wellness clinics have not undergone this rigorous scientific and regulatory scrutiny. They remain experimental, meaning their long-term effects, optimal dosages, potential side effects, and interactions with other medications are largely unknown. The distinction between scientifically validated, approved peptide medications and experimental, unregulated peptides is critical for public understanding and safety.
The MHRA’s Definitive Stance on Medicinal Products
The legal definition of a medicinal product in the UK, as enforced by the MHRA, is broad and encompassing. It includes "any substance or combination of substances presented as having properties of preventing or treating disease in human beings," where "disease includes any injury, ailment or adverse condition, whether of body or mind." Crucially, a product can also be deemed medicinal if it is "any substance or combination of substances that may be used by or administered to human beings with a view to restoring, correcting or modifying a physiological function by exerting a pharmacological, immunological or metabolic action, or making a medical diagnosis."
Lynda Scammell, the head of borderline products at the MHRA, elaborated on the agency’s approach: "Peptide products may be sold as cosmetics, supplements and medicines, and depending on their intended purpose, they fall under different regulatory frameworks." She emphasized the case-by-case nature of their assessments: "The MHRA determines whether a product is a medicine on a case-by-case basis. This includes consideration of a number of factors including the product’s effect on the body, the way it is used and takes into account all the available evidence and relevant legal precedents."
A key aspect of the MHRA’s enforcement strategy is its disregard for disingenuous labelling. Scammell unequivocally stated: "We disregard claims that products are for ‘research purposes’ if it is clear that such claims are being used as an attempt to avoid medicines regulations. If there is evidence within the promotional material that the products are in fact unauthorised medicines intended for human use, we will take appropriate regulatory action." This confirms the MHRA’s commitment to looking beyond superficial disclaimers to assess the true intent and impact of product promotion.
Broader Implications: Public Health, Ethics, and Regulatory Challenges
The MHRA’s investigation into experimental peptide therapies highlights several critical broader implications for public health, medical ethics, and regulatory enforcement in the digital age.
- Public Health Risks: The primary concern is the potential harm to individuals. Unregulated substances carry inherent risks, including unknown side effects, allergic reactions, interactions with other medications, and the danger of receiving contaminated or counterfeit products. Without rigorous clinical trials, consumers are essentially unwitting participants in uncontrolled experiments, with no guarantee of efficacy and significant potential for adverse outcomes. The financial cost to individuals, often hundreds of pounds monthly for unproven treatments, also represents a significant exploitation of consumer hope and vulnerability.
- Ethical Dilemmas for Medical Professionals: The involvement of some "medics" in promoting or administering these experimental therapies raises serious ethical questions. Medical professionals are bound by a duty of care and must practice evidence-based medicine. Recommending or providing treatments lacking robust scientific validation can breach professional codes of conduct and undermine public trust in the medical profession. Even with disclaimers about the experimental nature, the act of recommending specific peptides for therapeutic effects can be seen as tacit endorsement, leading patients to believe in their safety and efficacy.
- Regulatory Challenges in a Digital Landscape: The "boom" in interest is significantly driven by online promotion, including social media influencers and easily accessible clinic websites. This digital environment presents substantial challenges for regulatory bodies like the MHRA. Products can be marketed globally, and claims can spread rapidly, making enforcement a constant uphill battle. The tactic of labelling products "for research purposes" while simultaneously detailing therapeutic "results" is a common strategy to circumvent regulations, requiring constant vigilance and robust legal action from authorities. The clinic’s own statement about individuals accessing products through "unregulated channels" underscores the pervasive nature of this issue, but it also highlights the need for a stronger regulatory presence to ensure that even "regulated" clinics do not become conduits for unproven treatments.
- The Pursuit of Wellness vs. Scientific Rigor: The narrative surrounding experimental peptides often taps into a societal desire for quick fixes for complex health issues, anti-ageing solutions, and performance enhancement. This cultural trend, coupled with the allure of cutting-edge (but unproven) science, creates a fertile ground for the marketing of such therapies. It becomes crucial for both regulators and the media to continuously educate the public on the fundamental difference between legitimate scientific advancement and speculative, commercially driven claims.
The MHRA’s investigation marks a crucial step in reasserting regulatory control over a rapidly expanding and potentially hazardous segment of the wellness industry. Its outcome will likely set precedents for how experimental therapies are marketed and delivered in the UK, sending a clear message that medical claims for unproven substances will not be tolerated. This ongoing vigilance is essential to safeguard public health and uphold the integrity of medical practice against the tide of unregulated innovation.







